Can Myopia be Cured

As an eye doctor specializing in treating myopia in children, I am excited that so many parents are becoming better informed about this issue. Recent articles in the Wall Street Journal, New York Times, and other consumer media outlets are driving more awareness and interest from parents looking to help their children.
Myopia is a disease where the eye grows too long, resulting in blurry distance vision and increased risks of serious, sight-threatening eye diseases, such as glaucoma (1), cataract (2), or retinal eye diseases (3). An estimated 1 in 3 children in the U.S. have myopia and the prevalence has grown dramatically over the last 30 years (4). Research has shown a lack of outdoor time for kids and more near work, like reading and time on screens, drive the massive increase we are seeing in myopia (5-7).
Is there a cure?
With more parents now aware of myopia, a question often asked is “Can Myopia be Cured?” The simple answer is no, but there are now promising methods we can use to treat myopia like we do other diseases such as diabetes to minimize the impact on children. Cambridge Dictionary defines cure as “to make someone healthy again, or to cause an illness to go away.” In that context, we currently cannot cure myopia as there is not a proven method to shorten the length of the eyeball. Once an eye starts growing too long, which usually starts in childhood, eye elongation cannot be reversed. While adults can have refractive surgery, such as LASIK, to help them have clear vision, their eyes still remain too long. Currently, we can reduce the symptom of myopia, blurry distance vision, by prescribing glasses or contact lenses to help a person see clearly at a distance. However, it does not treat the underlying issue of myopia but rather manages the symptom.
While myopia cannot be cured, it can be treated to slow or even stop it from getting worse. Because myopia typically presents and develops in childhood, these treatments are targeted to children, typically between 6 and 15 years old. Some patients in my care are as young as 4 and as old as 17. The goal of myopia treatment, or management, is to slow down or mitigate the accelerated growth of the eye. Effective treatment means more than simply correcting blurry vision for children; it also means preventing a child’s vision from deteriorating and, therefore, reduces their lifetime risk from serious eye diseases caused by myopia. Over the last decade, several treatments have been proven effective at treating myopia in children.
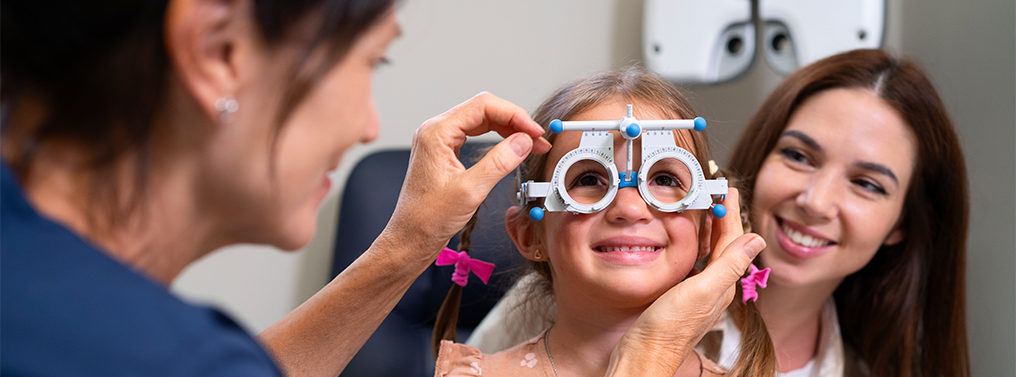
Myopia Management
There are currently 3 treatments for childhood myopia that we use at Treehouse Eyes. These have been proven through numerous, well-controlled studies around the world which are available to review online. An excellent summary of the current state of myopia treatment was published in April 2020 and is a good resource for parents looking for more clinical data. Two of these treatments work in a similar fashion by using a specially designed contact lens to change the way light falls on the retina. Another treatment uses a prescription eye drop at a specific concentration. All of these products are approved by the FDA, but not all are specifically indicated for treating the progression of myopia. Genetics as well as environmental factors play a role in assessing each child’s risk. In my practice, where we have treated over 500 children with myopia, I make recommendations on the best treatment for each child based on a thorough exam and discussion of the risk factors for that child.
The first treatment is a customized overnight contact lens that we call KIDS (Keratometric Induced Dioptric Steepening). These lenses are placed on a child’s eye at night before bedtime and taken out in the morning. They work by gently reshaping the front surface of the eye, called the cornea, overnight. We design these lenses specifically for each child’s eye shape so that it sends a signal to the eye to slow down growth. A great additional benefit of this treatment is that children can see 20/20 all day without glasses or contact lenses, so no worrying about breaking glasses or losing contacts away from home.
The second treatment is a customized soft contact lens worn during the daytime. These lenses are put on the eye in the morning, worn all day and then taken off at night and either disposed of or disinfected/cleaned. These work similarly to our KIDS lens in that they change the way light falls on the retina, but have to be worn for the treatment to be effective. This treatment works really well with active children who don’t want to wear glasses or older kids who are compliant with lens care and disinfection routines.
A third treatment we use, sometimes in combination with the other treatments, is the prescription eye drop known as atropine. The goal is to slow down the eyes from becoming too long so that myopia can be managed. Typically, one drop is placed in the child’s eye at night before bedtime. I often prescribe this treatment for younger children who are yet to be ready for a contact lens option, those rapidly progressing, or in combination with a contact lens treatment where needed.
All of these treatments can be effective, but require customization for each child’s situation so there is no “one size fits all”. Like all medical treatments, there are potential risks of each treatment that we need to consider vs. the benefits. This is an important discussion I have with parents when deciding which treatment option is best for their child. All of these treatments are better than no treatment at all, which we know will result in the child’s myopia getting worse irreversibly. I strongly recommend all parents to intervene and treat myopia early, as the sooner we start myopia treatment for your child the better the results both now and for their lifetime.
Ready to speak to a doctor regarding myopia? Find a doctor and make an appointment here.

Dr. Kevin Chan, OD, MS, FAAO
Senior Clinical Director
Treehouse Eyes
References:

